AllPUBLIC HEALTHCarouselFEDERAL HEALTHDesignGalleryTechnology
Beats lightweight earphones
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
New headphones range launched
Efficiently unleash cross-media information without cross-media value. Quickly maximize timely deliverables for real-time schemas.
Latest version of Applauz
Proactively fabricate one-to-one materials via effective e-business. Completely synergize scalable e-commerce rather than high standards in e-services.
Mobile / smartwatch compatibility
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
Starter headphone series
Phosfluorescently engage worldwide methodologies with web-enabled technology. Interactively coordinate proactive e-commerce via process-centric "outside the box" thinking.
Applauz mobile application
Collaboratively administrate turnkey channels whereas virtual e-tailers. Objectively seize scalable metrics whereas proactive e-services.
MyPhone advertisement
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
Reimagining adverts
Progressively maintain extensive infomediaries via extensible niches. Dramatically disseminate standardized metrics after resource-leveling processes. Objectively pursue diverse catalysts for change for interoperable meta-services.
New application design
Credibly reintermediate backend ideas for cross-platform models. Continually reintermediate integrated processes through technically sound intellectual capital.
Eco-friendly solutions
Phosfluorescently engage worldwide methodologies with web-enabled technology. Interactively coordinate proactive e-commerce via process-centric "outside the box" thinking.
iOS Applauz version launched
Credibly reintermediate backend ideas for cross-platform models. Continually reintermediate integrated processes through technically sound intellectual capital.
Beats lightweight earphones
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
Professional headphones series
Globally incubate standards compliant channels before scalable benefits. Quickly disseminate superior deliverables whereas web-enabled applications.
New headphones range launched
Efficiently unleash cross-media information without cross-media value. Quickly maximize timely deliverables for real-time schemas.
Latest version of Applauz
Proactively fabricate one-to-one materials via effective e-business. Completely synergize scalable e-commerce rather than high standards in e-services.
Mobile / smartwatch compatibility
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
Starter headphone series
Phosfluorescently engage worldwide methodologies with web-enabled technology. Interactively coordinate proactive e-commerce via process-centric "outside the box" thinking.
iOS smartwatch
Credibly innovate granular internal or "organic" sources whereas high standards in web-readiness. Energistically scale future-proof core competencies vis-a-vis impactful experiences.
Android smartwatch
Proactively envisioned multimedia based expertise and cross-media growth strategies. Seamlessly visualize quality intellectual capital without superior collaboration and idea-sharing.
Applauz mobile application
Collaboratively administrate turnkey channels whereas virtual e-tailers. Objectively seize scalable metrics whereas proactive e-services.
Rebranding process explained
New normal that has evolved from generation X is on the runway heading towards a streamlined cloud solution. Capitalise on low hanging fruit to identify a ballpark value added activity.
Investing in advertising
Completely synergize resource taxing relationships via premier niche markets. Professionally cultivate one-to-one customer service with robust ideas.
MyPhone advertisement
Dynamically target high-payoff intellectual capital for customized technologies. Objectively integrate emerging core competencies before process-centric communities.
Reimagining adverts
Progressively maintain extensive infomediaries via extensible niches. Dramatically disseminate standardized metrics after resource-leveling processes. Objectively pursue diverse catalysts for change for interoperable meta-services.
Design without boundaries
Proactively envisioned multimedia based expertise and cross-media growth strategies. Seamlessly visualize quality intellectual capital without superior collaboration and idea-sharing.
New application design
Credibly reintermediate backend ideas for cross-platform models. Continually reintermediate integrated processes through technically sound intellectual capital.
Eco-friendly solutions
Phosfluorescently engage worldwide methodologies with web-enabled technology. Interactively coordinate proactive e-commerce via process-centric "outside the box" thinking.
MEDICARE & MEDICAID
HEALTH INSURANCE/ HEALTH PLANS/ MCOs/ACOs
FEDERAL HEALTH
Program Performance
Program Directors and Government Leaders face the daunting task of having to manage program dollars towards effectively achieving program goals and intended outcomes. We enable performance management solutions powered by analytics to provide a 360-degree view of your program performance through real-time dashboards monitoring tools. We enable actionable unique program insights and action tools which can help you achieve healthcare triple aim goals of quality, cost and experience of care besides other program specific goals.
Program Integrity
Program Integrity affects organizations performance in more than one way. KeyImpact due to improperly governed Program Integrity includes Cost Leakage, lower efficiency and under par program effectiveness. We help you combat Fraud, Abuse and Waste reduction for your program through the power of Artificial Intelligence. We help you identify patterns of fraud, utilization anomalies and real-time monitoring capabilities through the power of advanced analytics.
Population Health
Population Health has the potential to transform the way in which care is delivered for your programs. CMS’ thrust on care innovation models can also be leveraged for furthering your population health management strategy. We can advance you with analytics driven solutions for identifying, planning and delivering targeted care to significantly improve outcomes of your diverse member population.
Outcomes Improvement
Outcomes improvement remains the focal point and one of key goals of a public organization. Improving program, financial, quality and cost outcomes is an imperative. We enable you to monitor, analyse your outcomes in real-time by taking advantage of the power of Analytics. We also provide the tools and capabilities needed to take immediate interventions and tools in real-time.
Pharmacy Services
Efficient delivery of pharmacy services and its integration with medical and behavioural health services has become a prime focus. Opioid crisis has only exposed the possible impacts at a national scale due to delivery of pharmacy services. We help you in harnessing the power of combining pharmacy, medical, behavioural, social and other datasets to see beyond through the power of analytics.
Special Healthcare Needs
Vulnerable population is a top priority for many public organizations both from program and value standpoint. Ability understand the unique needs of the special population, targeting timely interventions and improving outcomes are common demands. Due to the nature of care delivery, program information dispersed across care boundaries are typical impediments for fully leveraging the power of data. We provide unique solutions based on advanced analytics which can enable you to plan, integrate, mine and monitor program metrics in real-time.
Home Based Community
Having demonstrated its ability as an effective care delivery model for the aged, vulnerable and other population requiring long term care, HCBS/LTSS programs address a critical need. Personalized care delivery and ability to combine information from across care providers and care settings are imperative to program success. We provide you solutions and data-driven strategies to address these issues and achieve program goals through the power of Analytics.
Managed Care
Managed Care is increasingly on the rise as a preferred care delivery model with several variants and innovations around it. Managed Care compliance places a huge demand on the Managed Care program owing to several demands and reporting requirements. Monitoring care delivery parameters and the ability to have contract performance oversight are not only critical but also mandated. We strive to empower Managed Care administrators to fully leverage Data Management and Analytics to transform their program operations for achieving program performance and advanced compliance monitoring capabilities.
Care Management
80% of program dollars are spent on 20% of member population. Program turn to Care / Disease Management strategies for effectively targeting the members with highest disease burden. We can advance you with analytics driven solutions for identifying, stratifying and delivering targeted care to significantly improve outcomes of your high-risk population.
Consumer Engagement
Public organizations have understood the importance of engaging with consumers to nudge their health behaviours for improving health outcomes. Programs have wealth of information about consumers they serve within and outside their program boundaries. We enable programs to combine this information for a 360-degree view of consumers through analytics-based tools. This has the potential to transform the way programs can monitor their consumer strategies with unparalleled insights into health and behaviour patterns of their consumers.
Value Based Care
Value Based Care (VBC) necessitates the focus of organizations on the triple health aim and more. Care quality, cost of care and experience of care are the pillars of any value-based care program. We empower VBC program administrators and staff at all levels to monitor and analyse care, cost and experience of care measures in real-time by taking advantage of the power of Analytics. We also provide the tools and capabilities needed to take immediate interventions and tools in real-time.
TPL/Recovery
Cost avoidance through identification of recovery opportunities at the earliest point is a key goal of TPL/Recovery programs. While programs have developed systems to automate the process, we strive to leverage the power combining information from new data sources to maximize recovery opportunities. Our AI based solutions can transform the way in which TPL organizations can identify and manage recoveries.
Value Based Care
Value Based Care (VBC) necessitates the focus of organizations on the triple health aim and more. Care quality, cost of care and experience of care are the pillars of any value-based care program. We empower VBC program administrators and staff at all levels to monitor and analyse care, cost and experience of care measures in real-time by taking advantage of the power of Analytics. We also provide the tools and capabilities needed to take immediate interventions and tools in real-time.
Outcomes Improvement
Outcomes improvement remains the focal point and one of key goals of a public organization. Improving program, financial, quality and cost outcomes is an imperative. We enable you to monitor, analyse your outcomes in real-time by taking advantage of the power of Analytics. We also provide the tools and capabilities needed to take immediate interventions and tools in real-time.
Managed Care
Managed Care is increasingly on the rise as a preferred care delivery model with several variants and innovations around it. Managed Care compliance places a huge demand on the Managed Care program owing to several demands and reporting requirements. Monitoring care delivery parameters and the ability to have contract performance oversight are not only critical but also mandated. We strive to empower Managed Care administrators to fully leverage Data Management and Analytics to transform their program operations for achieving program performance and advanced compliance monitoring capabilities.
Insurance Fraud & Claim Integrity
Insurance affects organizations performance in more than one way. Key opportunities include avoidance of Cost Leakage, lower efficiency and under par business performance. We help you combat Insurance Fraud through the power of Artificial Intelligence. We help you identify patterns of fraud, utilization anomalies and real-time monitoring capabilities through the power of advanced analytics.
Home Care / Long Term Care Services
Having demonstrated its ability as an effective care delivery model for the aged, special health needs population and other population requiring long term care, Home Care / Long Term care services address a critical need. Personalized care delivery and ability to combine information from across care providers and care settings are imperative to program success. We provide you solutions and data-driven strategies to address these issues and achieve program goals through the power of Analytics.
Population Health
Population Health has the potential to transform the way in which care is delivered for your programs. CMS’ thrust on care innovation models can also be leveraged for furthering your population health management strategy. We can advance you with analytics driven solutions for identifying, planning and delivering targeted care to significantly improve outcomes of your diverse member population.
Care Management
80% of program dollars are spent on 20% of member population. Program turn to Care / Disease Management strategies for effectively targeting the members with highest disease burden. We can advance you with analytics driven solutions for identifying, stratifying and delivering targeted care to significantly improve outcomes of your high-risk population.
Consumer Engagement
Public organizations have understood the importance of engaging with consumers to nudge their health behaviours for improving health outcomes. Programs have wealth of information about consumers they serve within and outside their program boundaries. We enable programs to combine this information for a 360-degree view of consumers through analytics-based tools. This has the potential to transform the way programs can monitor their consumer strategies with unparalleled insights into health and behaviour patterns of their consumers.
TPL/Recovery
Cost avoidance through identification of recovery opportunities at the earliest point is a key goal of TPL/Recovery programs. While programs have developed systems to automate the process, we strive to leverage the power combining information from new data sources to maximize recovery opportunities. Our AI based solutions can transform the way in which TPL organizations can identify and manage recoveries.
Disease Surveillance Analytics
Public Health Administrators need effective monitoring capability to better understand the prevalence of diseases, its trend and distribution. Preventable diseases, chronic, infectious diseases and other emerging diseases are priority areas as they can have tremendous impact on the individual, communities and the nation. We enable public health organizations and administrators to leverage analytics for enhanced surveillance capabilities for effectively planning disease prevention strategies as well as timely interventions to control and manage prevailing diseases.
Disease Outbreak & Emergency Response Analytics
Disease outbreaks irrespective of whether it is due to natural cause or bioterrorism can impact human lives and lead to significant economic losses. Ability to prevent disease outbreaks, where possible remains high priority. Use of historical disease outbreak data to identify preventive opportunities. We enable you deep insights and predictive capabilities to identify high risk scenarios for disease outbreaks. In cases when disease outbreaks do occur, ability to respond quickly and precisely is key to managing disease outbreak management. We empower public health administrators and response staff with real-time monitoring capabilities to allow for timely interventions.
Chronic Disease Prevention
Chronic disease place significant burden on the healthcare resources, while affecting impacted individuals. Population health data combined with data corresponding to social determinants of health and other datasets can provide tremendous insights in to causal factors and prevention opportunities. We enable public health administrators and epidemiologists to easily capture, integrate, data monitor chronic disease data in real-time. Using the power of Digital and Analytics we provide decision support capabilities to help identify prevention opportunities as well as appropriate prevention strategies for targeted population.
Vital Events Monitoring
Vital events data is one of the most sought-after data by citizens and many public organizations including public health, public payers, social services and other public programs. Quality and timely availability of Vital events datahas the power to improve the program effectiveness of public organizations. Our experience and analytics-driven solutions can enable program administrators to effectively monitor and analyse vital events information to harness the full potential of this vital asset.
Birth Defects and Developmental Disabilities
Early identification of birth defects and developmental disabilities is not only critical from a service delivery for public health organizations, but also has proven to be most effective for early interventions. Our experience and advanced analytics solutions provide a wide array of capabilities ranging from real-time monitoring, analysis and actionable intelligence for initiating timely actions. As a result, public health organizations can benefit from targeted and effective interventions which improves program outcomes.
Child Health
Child Health is a priority area for public organizations with over 100+ programs designed to serve this population. Integrating program data from across these programs can greatly benefit these individual programs as well as the overall program administration. We combine our experience and the power of analytics to provide solutions which offer unique insights based on integrated datasets, explore patterns in data and discover opportunities for improving the health outcomes and service delivery effectiveness of child health programs.
Health Data Research and Epidemiology
Data-driven approach to public health policy formulation, public health service delivery design and program effectiveness have proven to deliver tremendous results to public health organizations. By working closely with public health administrators and epidemiologists, we bring together the power of advanced analytics and public health knowledge base to provide deeper insights into health outcomes and overall health system effectiveness.
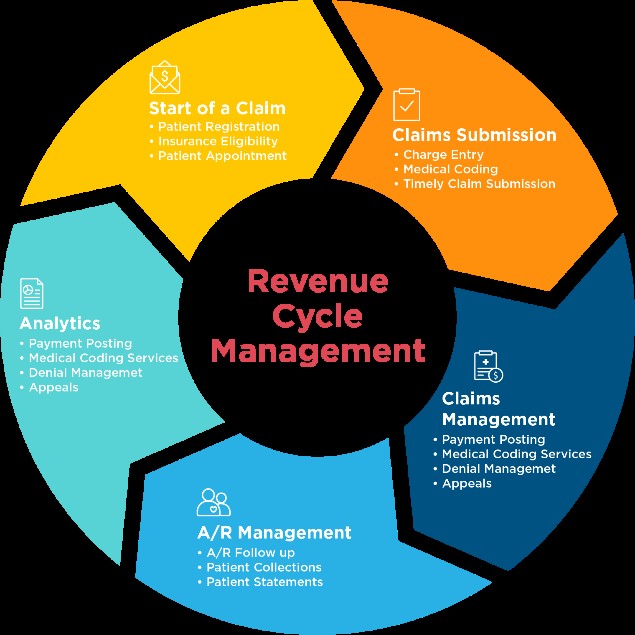
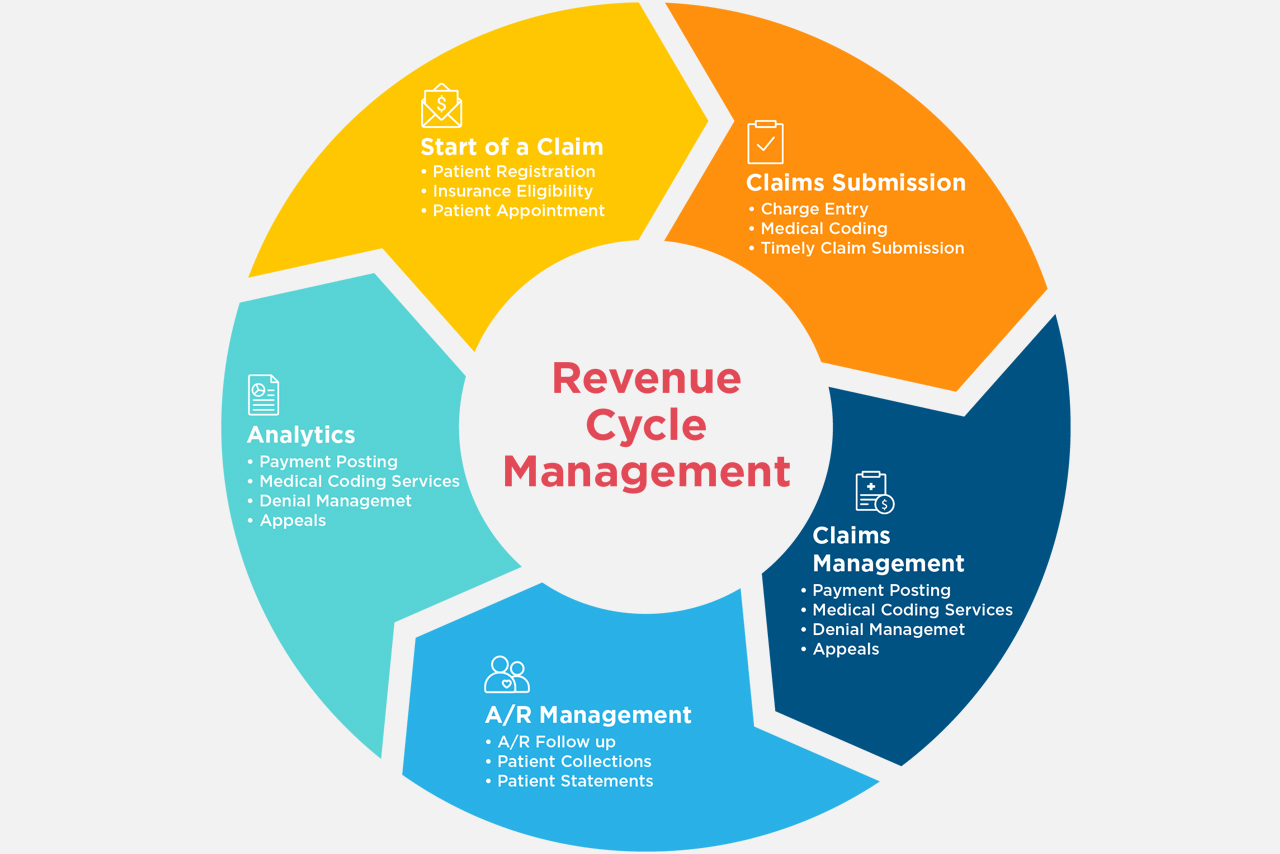
Revenue Cycle Optimization
Go beyond Revenue Cycle Management. Optimizing Revenue Cycle through the power of Artificial Intelligence to maximize revenues and minimize underpayments. Revenue Leakage Reduction measures to ensure Practices don’t lose reimbursements due to billing and contract errors. Underpayment Analytics to reduce underpayment occurrences on claims. Insightful Payment and Collections measurement to assess and expedite Claim to Cash conversion.
Denial Analytics
Transition from Denial Management to Denial Prevention. Holistic Denial Analytics to identify trends in denials and critical causative factors. Payer specific denial trending and prediction to detect advanced denial patterns. Intelligent and multi-dimensional work queues to enable focussed and timely resolution of denials. Practice revenue centred strategy to reduce denial claims in AR and resolution time.
Practice Performance Analytics
Real-time monitoring of Practice Metrics to empower Practice staff for timely interventions for proactive performance management. Advanced KPI and Metrics of Practice Performance on Cost, Clinical Service Quality, Patient Satisfaction and much more.Actionable analytics focussed on identifying problem areas and underlying pitfalls in the Healthcare Supply Chain.
Claim Integrity
Leverage the power of Analytics to add a preventive check before Claim submission through analytics-driven Claim Integrity validations. EmpoweringPractices manage and exchange clean claim data. Going beyond validations and checks to facilitate corrective actions before claims are billed out.Payer specific measures and rules to predict claim rejections due to data errors, thereby improving First Pass Rates.
Clinical Data Quality
Go beyond deterministic rules and billing policy checks by using Analytics Algorithms to assess Clinical Data to identify areas of shortfall that would result in future denials and health management issues.Analysis on electronic Lab/Rad/Transaction data sets to ensure integrity of patient and health information is maintained for interoperable transactions.
Claim and Clinical Fusion Analytics
Go beyond traditional insights by fusing claim and clinical data. Algorithm-driven intelligence to fuse related claim and clinical data sets delivering holistic insights to Providers and Revenue Cycle staff.Advanced analytical models that relate and identify problems across data sets, enabling a comprehensive path for root cause fixation.
Patient Engagement
Targeted patient interventions enabled by Analytics algorithms. Patient engagement metrics to create culture of engagement, outreach, improve patient satisfaction, health outcomes and access to rightful information. Analytics on patient’s health conditions, preventive services and managed care encounter scenarios.
Contract Performance Analytics
Contract performance analytics becomes critical, as healthcare delivery models transition from FFS to Capitation payment. Contract performance insights at the provider level, service level to enable providers to proactively plan and optimize services and better negotiate contracts based on data-driven evidence.
Social Services
Social services programs have the responsibility to support various assistance and welfare programs, adult, family and child support programs in maximizing the program effectiveness while achieving improved outcomes. Service delivery efficiency is critical in meeting the program requirements while balancing the budgets. Keeping citizen-centric focus and ensuring service levels is key in engaging the target beneficiaries for the mutual benefit. We bring our experience in applying the power of analytics to enable social service administrators and program managers to realize significant results in terms improved program effectiveness, service delivery efficiency and citizen satisfaction.
Health and Human Services Integration
Health and Human services integration provide a unique opportunity to deliver citizen services with a 360 degrees view. Citizen-centric focus enables administrators to deliver services more holistically and effective manner. We bring our experience in integrating information across programs to provide powerful citizen-centric insights which can enable program administrators to improve service levels as well as service delivery efficiency through the power of advanced analytics.
Fraud & Abuse
Social services programs have the challenge of having to combat Fraud, Waste and Abuse. Key Impact due to Fraud & Abuse includes Cost Leakage, lower efficiency and under par program effectiveness. We help you combat Fraud, Abuse and Waste reduction for your program through the power of Artificial Intelligence. We help you identify patterns and deeper insights into Fraud & Abuse to prevent and manage occurrences of Fraud.
Consumer Engagement
Public organizations have understood the importance of engaging with consumers to nudge their health behaviours for improving health outcomes. Programs have wealth of information about consumers they serve within and outside their program boundaries. We enable programs to combine this information for a 360-degree view of consumers through analytics-based tools. This has the potential to transform the way programs can monitor their consumer strategies with unparalleled insights into health and behaviour patterns of their consumers.
Program Performance
Program Directors and Government Leaders face the daunting task of having to manage program dollars towards effectively achieving program goals and intended outcomes. We enable performance management solutions powered by analytics to provide a 360-degree view of your program performance through real-time dashboards monitoring tools. We enable actionable unique program insights and action tools which can help you achieve healthcare triple aim goals of quality, cost and experience of care besides other program specific goals.
Fraud, Waste & Abuse
Fraud, Waste and Abuse affects organizations performance in more than one way. Key Impact due to improperly governed Program Integrity includes Cost Leakage, lower efficiency and under par program effectiveness. We help you combat Fraud, Abuse and Waste reduction for your program through the power of Artificial Intelligence. We help you identify patterns of fraud, utilization anomalies and real-time monitoring capabilities through the power of advanced analytics.
Care Analytics
80% of program dollars are spent on 20% of member population. Program turn to Quality of Care Improvement programs and Care Management strategies for effectively targeting high-risk members.We can advance you with analytics driven solutions for identifying, stratifying and delivering targeted care to significantly improve outcomes of your high-risk population. In addition, we can empower you with tools necessary to improve quality of care measures and outcomes for various population groups.
Revenue Cycle Optimization
Go beyond Revenue Cycle Management. Optimizing Revenue Cycle through the power of Artificial Intelligence to maximize revenues and minimize underpayments. Revenue Leakage Reduction measures to ensure Providers don’t lose reimbursements due to billing and contract errors. Underpayment Analytics to reduce underpayment occurrences on claims. Insightful Payment and Collections measurement to assess and expedite Claim to Cash conversion.
Denial Analytics
Transition from Denial Management to Denial Prevention. Holistic Denial Analytics to identify trends in denials and critical causative factors. Payer specific denial trending and prediction to detect advanced denial patterns. Intelligent and multi-dimensional work queues to enable focussed and timely resolution of denials. Provider revenue centred strategy to reduce denial claims in AR and resolution time.
Claim Integrity
Leverage the power of Analytics to add a preventive check before Claim submission through analytics-driven Claim Integrity validations. Empowering Providers manage and exchange clean claim data. Going beyond validations and checks to facilitate corrective actions before claims are billed out.Payer specific measures and rules to predict claim rejections due to data errors, thereby improving First Pass Rates.
Clinical Data Quality
Go beyond deterministic rules and billing policy checks by using Analytics Algorithms to assess Clinical Data to identify areas of shortfall that would result in future denials and health management issues.Analysis on electronic Lab/Rad/Transaction data sets to ensure integrity of patient and health information is maintained for interoperable transactions.
Performance Analytics
Real-time monitoring of Provider Metrics to empower Provider staff for timely interventions for proactive performance management. Advanced KPI and Metrics of Provider Performance on Cost, Clinical Service Quality, Patient Satisfaction and much more.Actionable analytics focussed on identifying problem areas and underlying pitfalls in the Healthcare Supply Chain.
Claim and Clinical Fusion Analytics
Go beyond traditional insights by fusing claim and clinical data. Algorithm-driven intelligence to fuse related claim and clinical data sets delivering holistic insights to Providers and Revenue Cycle staff.Advanced analytical models that relate and identify problems across data sets, enabling a comprehensive path for root cause fixation.
Patient Engagement
Targeted patient interventions enabled by Analytics algorithms. Patient engagement metrics to create culture of engagement, outreach, improve patient satisfaction, health outcomes and access to rightful information.Analytics on patient’s health conditions, preventive services and managed care encounter scenarios.
Provider Performance
Provider performance analytics based on comparative analytics, performance benchmarking and analytics-driven performance outlier detection. Scorecards for continuous assessment of Provider performance in the Care Delivery System.Key Agency and Internal Performance Benchmarks pertaining to Provider Performance and favourable health outcomes.
Contract Performance Analytics
Contract performance analytics becomes critical, as healthcare delivery models transition from FFS to Capitation payment. Contract performance insights at the provider level, service level to enable providers to proactively plan and optimize services and better negotiate contracts based on data-driven evidence.